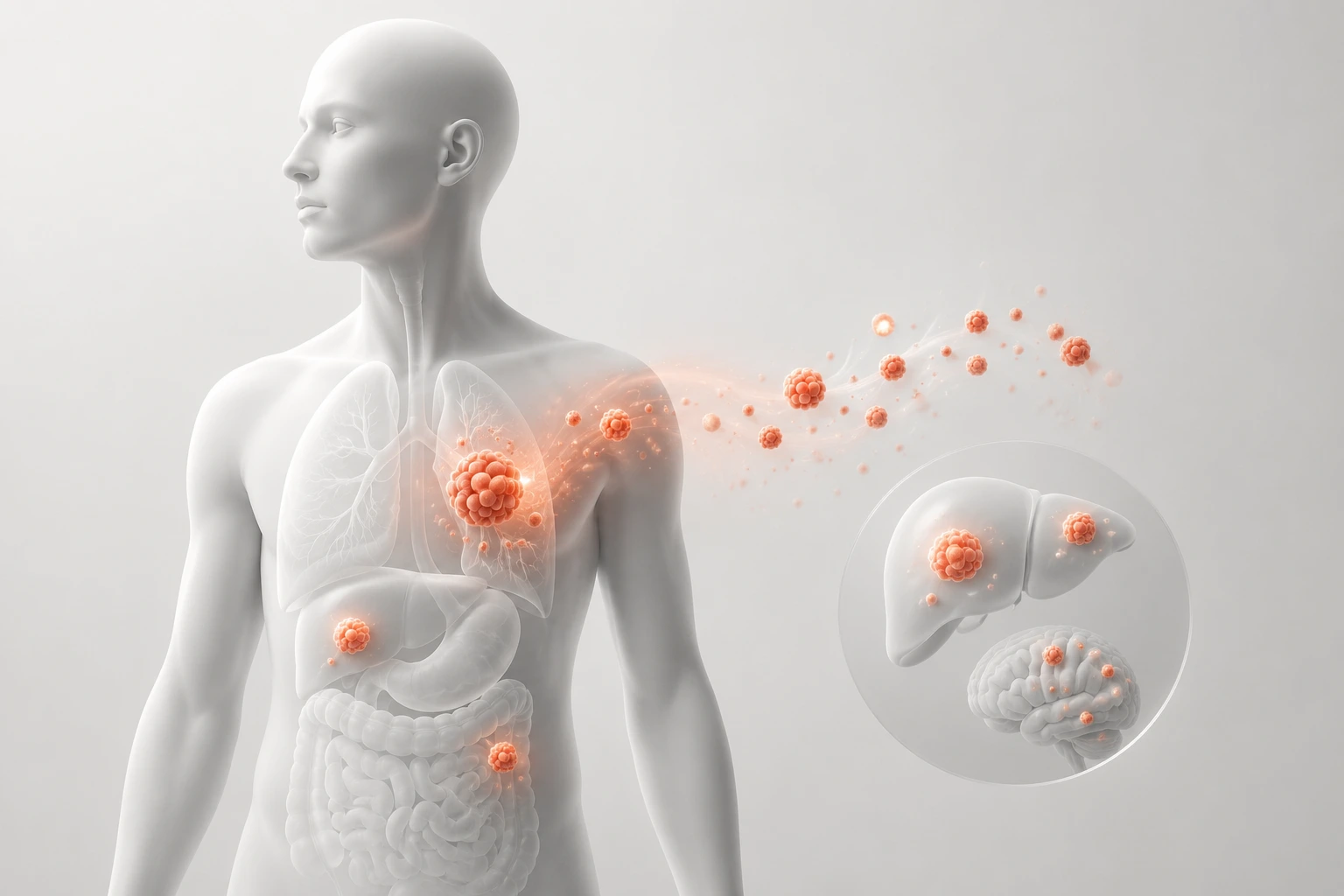
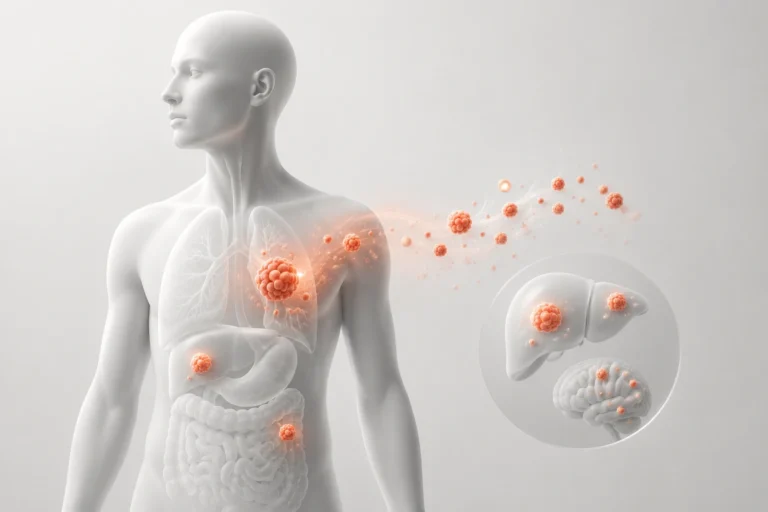
Metastatic cancer marks the stage where a localised tumour becomes a systemic, body-wide disease. Despite advances in early detection, immunotherapy, and precision medicine, metastasis is still responsible for the vast majority of cancer-related deaths globally.
In 2026, researchers increasingly describe metastatic cancer not as a single condition, but as an evolving biological system that adapts, resists treatment, and spreads through complex evolutionary processes inside the human body.
From Local Tumor to Systemic Disease
Cancer begins locally, but metastasis represents a fundamental shift in behavior. Primary tumors accumulate genetic mutations over time, and within that evolving mass, certain cancer cells gain aggressive traits that allow them to detach and spread.
Also Read:
- Tina Knowles; Mother of Superstar Singer Beyonce Reveals Battle With Breast Cancer
- After Cancer Scare, Waking Up To Soft Birdsong In Morocco - Olubunmi Ajai Layode
- Study: Drinking Up to Two Cups of Milk Daily Increases Risk of Breast Cancer in Women By Up to 80%
- Former US President Joe Biden Diagnosed With Prostrate Cancer
This transformation is driven by natural selection at a cellular level. The most adaptable cancer cells—those capable of surviving immune attacks, oxygen deprivation, and metabolic stress—are the ones most likely to metastasize.
Once this shift occurs, cancer is no longer confined to a single organ. It becomes systemic.
How Metastasis Cancer Spread Occurs
Metastasis follows a structured but inefficient sequence. Most cancer cells fail during this process, but the few that survive are highly resilient.
First, tumor cells lose adhesion properties, allowing them to break away from the primary tumor. They then invade nearby tissues and enter blood vessels or lymphatic channels in a process known as intravasation.
Once in circulation, cancer cells face extreme conditions. The majority are destroyed by immune defenses or shear stress in the bloodstream. Only a small fraction survive long enough to reach distant organs.
These surviving cells exit circulation (extravasation) and attempt to adapt to new tissue environments. If conditions are favorable, they establish secondary tumors.
This process can occur rapidly or remain dormant for years before reactivation.
Why Certain Cancers Spread to Specific Organs
Metastasis is highly pattern-driven rather than random. Cancer cells often spread to organs that provide compatible biological environments and receive significant blood flow.
Common patterns include:
- Breast cancer spreading to bone, liver, and brain
- Lung cancer spreading to brain and adrenal glands
- Colorectal cancer spreading to the liver
- Prostate cancer spreading primarily to bone
This behavior is explained by the “seed and soil” hypothesis, which suggests cancer cells (the seed) can only grow in suitable organ environments (the soil).
Symptoms Often Appear Only After Spread
One of the most dangerous features of metastatic cancer is its ability to progress silently. Many patients experience no symptoms until secondary tumors begin to disrupt organ function.
Symptom patterns depend on location:
- Bone metastasis: persistent pain, fractures, elevated calcium levels
- Brain metastasis: headaches, seizures, neurological decline
- Liver metastasis: jaundice, fatigue, abdominal swelling
- Lung metastasis: breathing difficulty, fluid buildup
Systemically, many patients develop cancer cachexia, a severe wasting syndrome driven by metabolic disruption and inflammation.
Diagnosis: Mapping a Systemic Disease
Diagnosis of metastatic cancer relies on imaging and molecular confirmation.
CT scans, MRI, and PET imaging are used to detect tumor spread, while biopsies confirm that secondary tumors originate from the primary cancer.
In 2026, liquid biopsy technologies are increasingly used to detect circulating tumor DNA, enabling earlier detection of relapse or progression.
Molecular profiling is also becoming standard, allowing oncologists to match treatments to specific genetic mutations within tumors.
Treatment: From Cure to Control
Once cancer becomes metastatic, treatment typically shifts from curative intent to disease control, although long-term remission is possible in select cases.
Systemic therapies form the backbone of treatment:
- Chemotherapy targets rapidly dividing cells across the body
- Targeted therapies block specific genetic drivers of cancer growth
- Immunotherapy reactivates immune system recognition of tumors
- Hormone therapy is used in hormone-sensitive cancers such as breast and prostate cancer
Local treatments like surgery or radiation are used selectively for symptom relief or isolated metastases.
In some cancers, particularly melanoma and lung cancer, immunotherapy has significantly improved long-term survival outcomes.
Why Metastatic Cancer is Difficult to Treat
Metastatic cancer is not a single uniform disease but a collection of evolving tumor populations across different organs.
Each metastatic site can develop its own genetic mutations, leading to drug resistance and treatment variability. Drug delivery barriers, such as the blood-brain barrier, further complicate treatment.
Additionally, metastatic tumors actively reshape their microenvironments, suppressing immune responses and promoting blood vessel formation to sustain growth.
This adaptability makes metastasis one of the most resilient biological processes in medicine.